Developing medicines
Developing medicines
Research into, and the development and production of, new therapies, medicines and vaccines are the core of Janssen's work. The improvement of patient care and its positive impact on society are always at the forefront of this. For example, we have launched 15 new medicines and vaccines on the market since 2012. And the WHO's list of essential medicines now includes 18 medicines developed by Janssen.1
Research into, and the development and production of, new therapies, medicines and vaccines are the core of Janssen's work. The improvement of patient care and its positive impact on society are always at the forefront of this. For example, we have launched 15 new medicines and vaccines on the market since 2012. And the WHO's list of essential medicines now includes 18 medicines developed by Janssen. However, our work does not end here. We are also working on innovative applications that help us use our new treatments in an increasingly targeted manner, and to diagnose or even prevent diseases even better and at an earlier stage. Our R&D campus in Beerse plays a crucial role in all these different areas.
What is drug research?
Improving the lives of patients in a sustainable way, that is our goal. How do we do it? By continuing to invest and innovate and by looking for solutions to the challenges of tomorrow. For example, Janssen has more than sixty years of research experience in mental health. The founder of our company, Dr. Paul Janssen, was committed to the search for solutions for patients with mental illness and to the promotion of neuroscience research. As early as 1958, he ushered in a new psychopharmacological era with the introduction of the first anti-psychotic treatments for schizophrenia. Neuroscience and its focus on neurodegenerative diseases and mental health continue to be a major focus of our research strategy.
We also try to make a difference within our other therapeutic areas. Janssen has been working on writing HIV history for more than 25 years. During this time, the company has developed nine new drugs for people living with HIV and we are working hard on a vaccine to prevent the disease.
Another important part of our R&D activities is within the field of oncological personalized medicine, where we focus on new treatment strategies for patients with the highest medical need in blood cancers and solid tumors.
However, drug research is not only the research done on new drugs or vaccines, but also, for example, on new methods of administration and biomarkers (a measurable indicator to quickly recognize certain conditions). Here we look not only at the curative effect but also for example at the impact of treatment on the daily life of the patient. Improving the quality of life through medication is an important factor that is receiving more and more attention. For example, the world's first fully long-acting injectable treatment regime was developed in Belgium with our cooperation and is now used as a form of administration throughout our therapeutic areas. Janssen was the first to develop such a regime for HIV, as a result of which patients only receive treatment six or twelve times a year instead of every day.2
Furthermore, the research also encompasses all activities that are performed after a drug, therapy or vaccine has become widely available. In this way, we are constantly looking to see whether we can improve the use of the treatment and analyze the results from daily clinical practice. You can read more about this in Chapter 8.
The phases of drug development: from lab to patient
The path a molecule takes from the moment of its discovery in the lab to its application in a new treatment is long and uncertain. At Janssen, we currently have more than 100 candidate drugs and vaccines in various stages of development, but a significant proportion of these (in their current form) will ultimately not make it to the finish line. This can happen because of several reasons, such as efficacy being too low or patient burden being unacceptable. On average, the development of a new, innovative treatment takes about 12 to 13 years. Several phases can be distinguished in this research process, all of which must, of course, be successfully completed.
Discovery phase
The development of new therapies, drugs or vaccines starts with a better understanding of the biological processes at the origin of disease, and of the molecular and genetic composition of pathogens, the particles that generate disease. Much of this work in the discovery phase is carried out by academic researchers or biotechnology start-ups outside Janssen with whom we collaborate. Thanks to our constant focus on innovation, we are able to find new starting points for treatments and develop them further. These starting points are very diverse. They range from developing small molecules in medications, to developing biological treatments that use natural proteins, or cellular therapies that use the immune system to fight malignant cells.
From lab to patient
The process of research and development


Dirk De Smaele
Global Head Chemical and Pharmaceutical Development & Supply
Translational research and preclinical research
More knowledge about the origin and progression of diseases often finds its origin in basic scientific research. This involves research into the mechanism that causes a disease or the genetic composition of a virus. By carrying out translational research, we try to convert this fundamental knowledge and recent discoveries about the disease into practical applications. So it is literally a search for possible ways to help patients: can we intervene in the mechanism that causes the disease? What part of the genetic code of a virus is suitable to develop a vaccine with? In this phase, we use our experience and knowledge to develop new molecules, antibodies, cell therapies or vaccines.
Next, the phase of so-called preclinical research begins. In this phase, the dosage, safety and effectiveness of the candidate drug or vaccine are investigated thanks to the use of models. These can be in vitro models, cell cultures, computer models and laboratory animals. Based on these results, our research teams decide whether a potential new treatment is safe and effective enough to also investigate in humans. Because patient safety is always paramount, many candidate treatments are already stranded at this stage.
Clinical and real-life research
When a drug or vaccine has successfully passed the preclinical phase, the effect of the drug on humans is investigated in a highly controlled environment. This phase is called clinical trials, which determine whether the new treatment is sufficiently effective and has an acceptable safety profile. You can read more about this in Chapter 4. The ultimate goal, after completing successful clinical trials, is to submit an application to the European Medicines Agency, or EMA, to allow the drug, therapy or vaccine to enter the market based on all of our research data. After going through the national pricing and reimbursement procedure in close consultation with the competent authorities (seeChapter 6), the innovative treatment can then be used in everyday practice. In exceptional circumstances, such as a major medical emergency, certain medical innovations can be administered even before the procedure is completed.
Our research does not stop when a drug or vaccine reaches the market. On the contrary, when a new treatment is used in everyday practice, we continue to work on solutions to make the drug even more effective. You can read more about this in chapter 8.
€ 8.44 Billion
In 2020, Janssen invested € 8.44 billion ($9.7 billion) worldwide in research and development. This amount has increased significantly in recent years. A significant proportion of this investment - more than 23% - is being made in our country.
1 in 10
One in 10 (9.6%) of our drug candidates entering phase 1 clinical trials will ultimately become available to patients. Thus, not every treatment makes it to the final stage.
Drug development itself is also in progress

Drug development is a lengthy and complex process. The fact that not all activities lead to the hoped-for result does not mean that the time and effort we have put into the research has been in vain. Even with research that does not immediately lead to a new treatment, we gain more knowledge about diseases and how we can combat them even better in the future. This acquired knowledge and expertise feeds the next steps in further development and is an important and inherent part of our innovation cycle.
More focused and complex
As our understanding of diseases improves, new treatments can be tailored increasingly to individual patients. We call this "personalized care". This method involves looking at a treatment that is ineffective in certain groups and where a tailored approach is needed. This makes treatments not only more efficient but also more complex. For example, with this type of treatment, there are fewer patients eligible to participate in clinical trials, which makes the research and production process more challenging. In addition, new treatments increasingly consist of biological drugs, gene therapy or cell therapy. These methods are more sophisticated than traditional medicines and are developed from biological substances or the body's own cells.
Prevention and interception
An important evolution within Janssen R&D is the evolution towards more prevention and timely interception of diseases. The underlying idea is that, thanks to medical evolution, we no longer need to focus solely on the (continuous) treatment of the disease affecting patients, but that we can also cure them or prevent them from becoming ill. From care to cure. In addition to the development of innovative vaccines, this applies not least in those areas where for the time being there are no conclusive or curative treatments available, such as cancer, autoimmune disorders and chronic inflammatory diseases. This new reality is already unfolding today with revolutionary therapies such as cell and gene therapy, but also thanks to the evolution in the application of artificial intelligence and big data.

The technology behind our vaccines

The technology behind our vaccines
At Janssen, we devote a great deal of attention to research into infectious diseases and the development of medicines and vaccines against these diseases. We do this from various expertise centers, including Janssen in Beerse and Janssen Vaccines in Leiden in the Netherlands. We conduct research into vaccines against various infectious diseases, such as respiratory syncytial virus (RSV), HIV, Ebola, zika, Methicillin-resistant Staphylococcus aureus (MRSA) and COVID-19. In some of our vaccines, we use our vaccine technology platform AdVac®. Because we have invested in this technology in recent years and were able to realize its application for our vaccine against Ebola, this helps us to develop new vaccines - for example against COVID-19 - faster.

Oligonucleotides

Oligonucleotides
Oligonucleotides are synthetically manufactured short strands of DNA and RNA. They have great potential as a therapy for various diseases because they can "control" the expression of genes in a cell. We strive for the campus in Beerse to become a global center of excellence in this field. Investments in R&D thus lead to the attraction of top talent, but also have a positive impact on our production and distribution capacity, for example.

COVID-19: Cooperation with the KU Leuven REGA Institute

COVID-19: Cooperation with the KU Leuven REGA Institute
We are cooperating with the REGA Institute of the KU Leuven in order to develop a treatment against COVID-19. We do this by screening existing drugs for their efficacy against the coronavirus. We started this collaboration at the same time as developing the COVID-19 vaccine. Vaccines help prevent illness and reduce the spread of the virus, but they do not provide a solution for people who have already become ill. So in this collaboration, we are screening existing molecules of all known drugs for antiviral activity against SARS-CoV-2, the virus that causes COVID-19. In this way, we want to identify a drug that has the potential to be converted into a new treatment for the virus, also called drug repurposing. Furthermore, we are also screening for new molecules and doing additional research on virus-neutralizing antibodies.
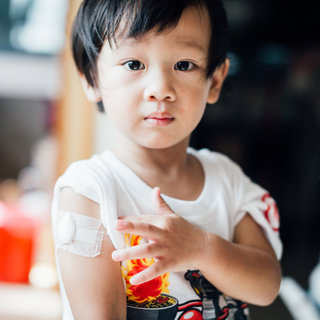
SDG 3: Good health and well-being
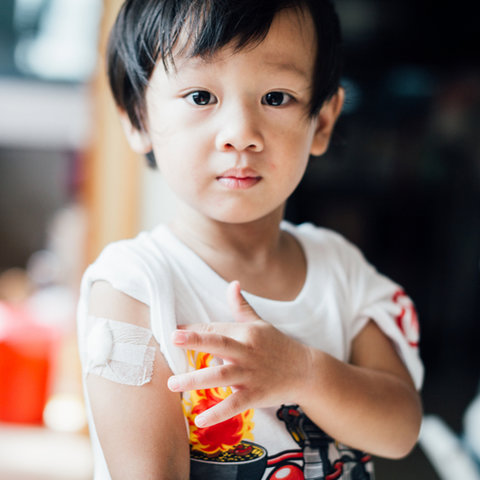
SDG 3: Good health and well-being
For more than 90% of our drugs that are in phase 2 clinical trials or beyond, we have developed plans to be able to make this drug available in lower and middle-income countries.3 Making our transformational treatments widely accessible is at the core of the mission and activities of Global Public Health, our end-to-end organization that works every day to address the health challenges that primarily affect lower- and middle-income countries (see also Chapter 7). We do this because we believe that the right to good healthcare applies to everyone, everywhere in the world.
We are therefore proud that our commitment to this theme has already been recognized with a top 3 spot in the Access to Medicines index since 2012. This index looks at the activities of the 20 largest pharmaceutical companies in researching the highest priority disease areas (according to WHO) and their strategies to then make these medicines accessible to all.
100+
Drug candidates currently under development at Janssen worldwide.
1,680 additional participants
In 2021, Janssen will have more than doubled the number of participants in our clinical development programs. For example, 37 new study protocols were set up at 72 different sites in Belgium (out of a total of 237 active studies). This led to 1,680 new participants out of a total of 2,565. The accelerated research into our vaccine is the main explanation for this.
Data sciences
A new tool in the research and development of innovative treatments is the use of artificial intelligence and data sciences. We use large data sets, machine learning and algorithms in all phases of drug development whenever possible. For example, we are trying to use data in a smart way to better understand the early stages of the onset of disease. Based on this, we are looking for clues to intercept diseases at this early stage. In doing so, we work with partners from academia and industry, and biotech partners to accelerate fundamental and translational research by using data science.
Even after a new therapy or drug is approved by the competent authorities, we can continue to use data science. For example, apps, wearables and sensors allow doctors to monitor patients remotely and use new treatments in an even more targeted way based on collected data and outcomes from daily practice, so-called 'real world data'. Measuring the outcomes and results of our new therapies and medicines is also important in terms of the agreements we are making with governments to make these innovative developments available to patients as quickly as possible. You can read more about this in Chapter 6 and Chapter 8.
Sources
- https://www.who.int/groups/expert-committee-on-selection-and-use-of-essential-medicines/essential-medicines-lists
- https://www.janssen.com/emea/sites/www_janssen_com_emea/files/janssen_receives_positive_chmp_opinion_for_long-acting_regimen_for_the_treatment_of_hiv.pdf
- https://accesstomedicinefoundation.org/publications/2021-access-to-medicine-index p.172


